Association between vaginal bleeding in pregnancy that resulted in delivery and risk of cancer– a Danish registry-based cohort study
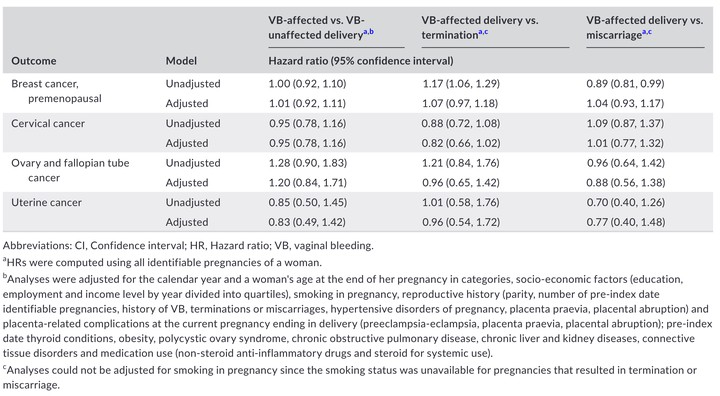 Highlighted results
Highlighted results
Abstract
Vaginal bleeding (VB) before 20 gestational weeks of a viable pregnancy is a manifestation of a threatened miscarriage. VB is associated with increased levels of pro-inflammatory cytokines such as interferon-gamma, tumour necrosis factor-alpha and interleukin-6. Increased levels of these cytokines and oxidative stress are risk factors for cancer. The risk of cancer following a VB-affected pregnancy that ended in childbirth is unknown. Objectives To investigate the associations between VB in pregnancy that resulted in delivery and risk of incident cancer. Methods - We conducted a cohort study (1995–2018) in Denmark using administrative and healthcare registries. We included 37,082 VB-affected deliveries, 1,363,614 VB-unaffected deliveries, 324,328 pregnancies ending in terminations, and 137,104 miscarriages. We computed the absolute risk of cancer and hazard ratios (HR) with 95% confidence intervals (CI) adjusted for age, calendar year, morbidities, and socio-economic factors using Cox proportional hazards regression. Multiple pregnancies to the same woman were accounted for in the analysis. Results The median (25th–75th percentile) follow-up in the study was 12.6 (6.9, 18.2) years. The prevalence of VB in the present study was 3%. At the end of the follow-up, there were 1320 cancer cases among the VB-affected delivery cohort, 40,420 among the VB-unaffected delivery cohort, 10,300 among the termination cohort and 4790 among the miscarriage cohort. HRs for any cancer among VB-affected deliveries were 1.03 (95% CI 0.97, 1.08) compared with VB-unaffected deliveries, 1.03 (95% CI 0.97, 1.09) compared with terminations and 0.90 (95% CI 0.84, 0.95) compared with miscarriages. There were no increased risks of premenopausal breast cancer, cervical cancer, ovary and fallopian tube cancer or uterine cancer following VB-affected deliveries vs. comparison cohorts. Conclusions We found no evidence of an association between vaginal bleeding in pregnancy and an increased risk of cancer.